Noninvasive Risk Stratification Using Microvolt-Level T-Wave Alternans,
Non-Sustained Ventricular Tachycardias and Autonomic Tone in MADIT-II-Type
Patients
Thomas Klingenheben MD,
Gerian Groenefeld, Pawel Ptaszynski, Stefan H. Hohnloser, J.W. Goethe University
Frankfurt, Frankfurt, Germany.
Background: Primary prevention of sudden
cardiac death (SCD) by prophylactic ICD implantation has been shown to be
effective in CAD patients with LVEF£30%. However, only one fifth of the respective
patients will use the ICD during follow-up. Refinement of risk stratification
of MADIT-II-like patients is therefore mandatory. Methods: Patients after
myocardial infarction and a LVEF£30% underwent assessment of microvolt T-wave alternans (TWA; spectral method), non-sustained
ventricular tachycardia (nsVT), and heart rate variability (HRV, both derived
from Holter recordings). The composite primary endpoint was SCD, sustained
ventricular tachycardia, and resuscitated ventricular fibrillation. Results:
One-hundred and sixteen patients (58±11 years; 81% males; LVEF 26±4%) were followed
over 27±17 months during which time period 12 primary endpoint
events (10%) occured. A positive TWA was found in 44 pts (38%), TWA was
negative in 31 and indeterminate in 41 pts. Twenty-one pts (18%) had nsVT
during Holter monitoring, HRV was impaired in 53 pts (46%). Only a positive TWA
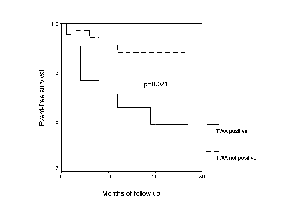
(RR 3.27; 95%CI:1.1-9.6; p=0.03) and the combination of TWA and nsVT (RR 5.66;
95%CI:2.1-14.9;p<0.001) were significant predictors of the composite
endpoint. The graph depicts Kaplan-Meier-Analysis of event-free survival.
Conclusion: TWA alone and in combination with nsVT identifies a subgroup of
MADIT-II like pts at particularly high risk for ventricular tachyarrhythmic
events. A prospective study of primary prevention of arrhythmic death in such
patients stratified by means of TWA is warranted.